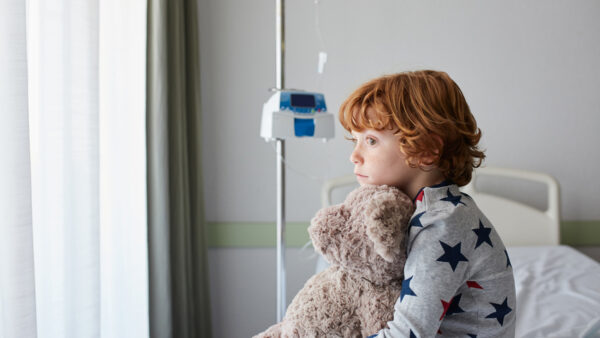
As the world turned upside down, people in every country were forced to grapple with unprecedented isolation, fear, anxiety, loss of work, illness, children learning at-home, and more. According to studies published in JAMA Network, binge drinking quickly became a coping mechanism for many:
“As stay-at-home orders began in some US states as a mitigation strategy for coronavirus disease 2019 (COVID-19) transmission, Nielsen reported a 54% increase in national sales of alcohol for the week ending March 21, 2020, compared with 1 year before; online sales increased 262% from 2019. Three weeks later, the World Health Organization warned that alcohol use during the pandemic may potentially exacerbate health concerns and risk-taking behaviors…
Comparisons before and during the COVID-19 pandemic were made on number of days of any alcohol use and heavy drinking (defined as 5 or more drinks for men and 4 or more drinks for women within a couple of hours), and average number of drinks consumed over the past 30 days. The 15-item Short Inventory of Problems assessed adverse consequences associated with alcohol use in the past 3 months (eg, “I have taken foolish risks when I have been drinking”). Comparisons were made overall, and across self-reported sex, age, and race/ethnicity. Significant changes were assessed based on whether the 95% CI around change from wave 1 to wave 2 included 0. Analyses include weights…
On average, alcohol was consumed 1 day more per month by 3 of 4 adults. For women, there was also a significant increase of 0.18 days of heavy drinking (95% CI, 0.04-0.32 days), from a 2019 baseline of 0.44 days, which represents an increase of 41% over baseline. This equates to an increase of 1 day for 1 in 5 women. For women there was an average increase in the Short Inventory of Problems scale of 0.09 (95% CI, 0.01-0.17 items), over the 2019 average baseline of 0.23, representing a 39% increase, which is indicative of increased alcohol-related problems independent of consumption level for nearly 1 in 10 women…
In addition to a range of negative physical health associations, excessive alcohol use may lead to or worsen existing mental health problems, such as anxiety or depression, which may themselves be increasing during COVID-19. The population level changes for women, younger, and non-Hispanic White individuals highlight that health systems may need to educate consumers through print or online media about increased alcohol use during the pandemic and identify factors associated with susceptibility and resilience to the impacts of COVID-19…”
A poll of 200+ Sermo physicians revealed similar findings.
When asked which substances they have seen an increase of use among patients, this is how the physicians responded:
- 52% said Alcohol
- 26% Benzodiazepines, such as Xanax
- 13% said Marijuana
- 5% said Prescription opioids
- 2% Prescription stimulants, such as Adderall
- 0% Cocaine
Regarding the long-term health health effects of increased alcohol and drug use, 69% of physicians said the biggest burden on physicians and hospitals will be emotional and mental health issues; and 25% said diseases rising from abuse (heart, liver, kidney etc.)
In addition, 77% said healthcare systems do not offer sufficient educational information and resources to help patients cope with the increase in stress and anxiety that the pandemic has caused. And 63% believe there has also been an increase of alcohol and drug use among healthcare workers.
Even when the pandemic is behind us, 66% of physicians believe that unhealthy increases in alcohol and drug use will persist as long-term coping mechanisms. See below for a quick recap of our findings:

Below, Sermo physicians from around the world share their professional insights, perspectives, and opinions on this important topic—in their own words:
Alcohol excess could increase domestic violence, falls + fractures, drunk driving, hypertensive crisis, foster overweight, noncompliance in treatment for chronic diseases (like diabetes/hypertension), in some individuals suicide increase, etc. (etc)
Oncology
Health systems do not face the reality representing the consequences of confinement by the pandemic. Depression, psychosis, anxiety, dependence to alcohol and drugs. It is necessary to implement a system of care for affected patients from the psychological point of view.
General Surgery
Easy access and addiction behind closed doors. Also financial stress from job loss, increased domestic violence, limited socialization opportunities in lockdown.
Pediatrics (excluding surgery)
Alcohol consumption, especially among women of child-bearing age may increase the incidence of ‘Feta-alcohol syndrome and ‘Feta-alcohol effect’ These are preventable cause of mental handicaps in children, and the latter is difficult to diagnose without history, often resulting in anti-social behavior in these children. This is in addition to an increase in automobile accidents, & other illnesses!
Pediatrics (excluding surgery) – Neonatal & Perinatal Medicine
In Germany alcohol is drug no. 1.
Gastroenterology
Everyday thousands of Sermo member physicians from diverse backgrounds and experiences exchange knowledge with each other. Sermo is the original medical social network that empowers today’s physicians. Over 1 million fully verified physicians across more than 150 countries come to our platform to talk with peers, participate in paid medical studies, solve challenging patient cases, contribute to the world’s largest database of drug ratings – and enjoy a few laughs along the way.
Interested in more? Check back any time and follow us on Facebook, Twitter, and LinkedIn for the latest and greatest in physician insights.
Are you a physician or healthcare practitioner? Explore the many benefits of joining Sermo’s medical community and sign up for free today.