High demand for Plasma and Remdesivir
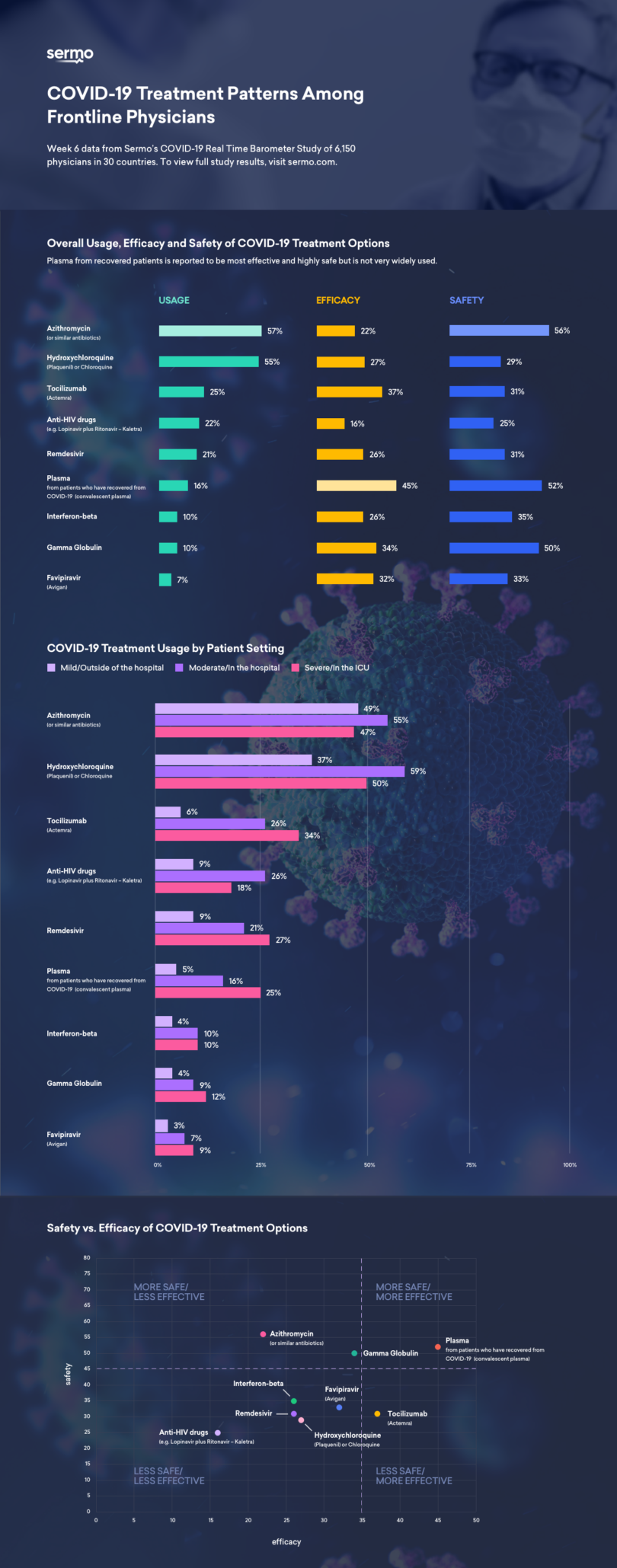
Currently, 55% of global physicians use Hydroxychloroquine, 24% use Tocilizumab, 21% use Remdesivir, 17% use Plasma
New York – May 7, 2020 – Week 6 results from Sermo’s COVID-19 Real Time Barometer with 6,150 physicians reveals COVID-19 treatment patterns among frontline physicians. In total, Sermo’s Barometer study includes over 33,700 survey interviews in 31 countries including the United States, Canada, United Kingdom, France, Brazil, Russia, China, Japan and Australia. Complete data published to date and study methodology can be found here.
Evaluations of COVID-19 treatments demonstrate that physicians have yet to find a universally effective solution; no treatment achieves a majority of physicians rating it as highly effective, with most garnering between 16% to 37% highly effective scores. The one exception is Plasma, which finds 45% of physicians rating it as highly effective. Remdesivir and Hydroxychloroquine are perceived as almost equally safe and effective.
Further evaluations of safety reveal additional challenges, as most physicians view commonly used treatments as not highly safe; though, we suspect safety of approved drugs is lower in the context of COVID-19 complications and comorbidities. Plasma and Gamma Globulin stand out, as over half of physicians rate them as highly safe.
Remdesivir and other antivirals
- Overall usage: Globally, 21% of physicians report having used Remdesivir, with a larger share of physicians (27%) using it within the ICU as opposed to just 9% of physicians using Remdesivir among mild patients.
- Geographic usage: 23% of physicians report using Remdesivir in the U.S., which is less than in Italy (31%), China (30%) and Germany (29%).
- Usage over time: The share of physicians using Remdesivir has nearly doubled from Week 1 to Week 6, rising from 12% the week of March 25 to 21% the week of April 28.
- Efficacy: Overall, 29% of physicians feel that Remdesivir is highly effective.This level remains consistent across settings (mild outside hospital/moderate-severe inside hospital/critical in the ICU).
- COVID-19 Supertreaters (highly experienced physicians who have treated 20+ COVID patients) feel it’s even less effective – only 18% of doctors feel it’s highly effective.
- One interesting point is that a significantly lower share of physicians perceive Remdesivir as less “highly effective” in the US (18%) vs the rest of the world (30%).
- Safety: Only 31% of physicians feel Remdesivir is highly safe.
Notes on other antivirals:
- Favipiravir is generally felt to be as effective and as safe as Remdesivir, however, only 7% of physicians report having used it.
- Acyclovir: Overall, only 7% of physicians have reported using it, with 13% rating it as highly effective (though 30% of physicians in the ICU consider it highly effective); Acyclovir has a higher perceived safety profile (35% feel it to be highly safe).
- Anti-HIV drugs (e.g. Lopinavir plus Ritonavir – Kaletra): 22% of physicians report using them globally, 16% rate them as highly effective, and 25% rate them as highly safe. Usage has declined from 30% (Week 4) to 23% (Week 5) to 22% (Week 6). Efficacy has also trended downward (23% to 17% to 16% in the last 3 weeks).
- Oseltamivir (Tamiflu) is used by 14% of physicians globally. Only 18% of physicians feel it to be highly effective, and they also rated Tamilfu as the one of safest drugs (58% rate it as highly effective).
Plasma and Gamma Globulin
- Overall usage: 16% of physicians report having used Plasma.
- Usage over time: Plasma usage has almost tripled with a 10 point increase since Week 1 and a 4 point since last week. Plasma usage in the ICU has grown the most, showing a close to 60% increase (16% in week 4 to 25% in week 6).
- Geographic usage: Usage is higher in the U.S. (22%) vs the rest of the world (14%) (~50% more physicians using in the U.S. vs globally).
- Efficacy: Overall, 45% of physicians feel that it is highly effective, and the results are consistent across settings (mild outside hospital/moderate-severe inside hospital/critical in the ICU).
- Safety: Plasma is still rated as one of the safest treatment alternatives with 52% of physicians rating it as highly safe.
“Convalescent plasma would be useful in certain stages of the disease, less so in others. It certainly has more scientific basis and potential than most of the options that have been loosely tested under anything but controlled conditions.” Sermo member, Emergency Medicine Physician, United States
Gamma Globulin is a protein fraction of blood plasma that responds to stimulation of antigens, as bacteria or viruses, by forming antibodies. It’s administered therapeutically in the treatment of some viral diseases.
- Gamma Globulin is starting to see the same usage trajectory as well as safety and efficacy perceptions as have been seen with plasma over the past three weeks. (7% in week 4, 6% in week 5 and 16% in week 6)
- 34% of physicians feel Gamma Globulin is highly effective (compared with 44% for plasma) and 50% felt Gamma Globulin to be highly safe as compared to 52% for plasma.
Tocilizumab
- Overall usage: 25% of physicians report using Tocilizumab, with higher usage seen in the ICU (34%).
- Usage over time: We see a 6-point increase in usage over the last two weeks. Usage has been increasing gradually with 19% of physicians having used Tocilizumab in Week 4, vs 25% in Week 6.
- Efficacy: Overall 37% of physicians feel that Tocilizumab is highly effective.
- Geographic usage: Usage in the U.S. is lower than around the globe, with 17% of physicians reporting they use it in the U.S. vs. 28% internationally. Physicians in Italy and Spain had the highest reported usage.
- Safety: 31% of Physicians rate Tocilizumab to be highly safe.
Hydroxychloroquine
- Overall usage: In Week 6, Hydroxychloroquine is still the most widely used drug following Azithromycin.
- Globally 55% of physicians report using Hydroxychloroquine. Its use in various settings breaks down as follows: 37% of physicians prescribe it outside the hospital for mild cases, 59% for moderate cases when patients get into the hospital, and 50% in the ICU.
- Usage over time: We see a 22-point increase in use from Week 1. Usage from Week 1 to Week 6 has increased significantly with 33% of physicians having used Hydroxychloroquine in Week 1 vs. 55% in Week 6.
- Geographic usage: Usage around the world varies widely; in the U.S., 46% of physicians report using it; that is significantly lower than other countries such as Italy (83%), Spain (78%), Mexico (76%), Brazil (85%), and China (62%). Usage in Great Britain is much lower at 19% and Germany at 13%.
- Efficacy: Globally 27% of physicians feel that it is highly effective. However, it is felt to be more effective outside of the hospital in mild-symptom patients (32%). This trend follows what we see in usage (higher usage in mild patients).Efficacy perceptions for Hydroxychloroquine were higher in Week 1,where physicians perceived it as the most highly effective drug.
- Safety: Despite being ranked as one of the least safe drugs (29% of physicians rated it as highly safe), it is still widely used.
Ideal vs. actual usage
A significant finding was that not all hospitals have access to all treatments they would like to use. We asked physicians which treatments they would use if they had access to any treatment – and the two treatments we saw clear demand for were Remdesivir and Plasma.
Overall, 41% of physicians would use plasma if it was an option – a significant 25% gap from the 16% who currently use it. The gap is exceptionally large among physicians treating patients in the ICU – 52% would use plasma if available, while just 25% are actually using it.
Remdesivir has a similar “demand gap,” with 39% of physicians saying they would prescribe Remdesivir (compared to 21% currently doing so). The gap is widest among physicians treating moderate/severe patients in the hospital, with 34% saying they would like to use it, compared to 16% that actually use it.
About Sermo
Sermo is the largest healthcare data collection company and social platform for physicians, reaching 1,3MM HCPs across 150 countries. The platform enables doctors to anonymously talk real-world medicine, review treatment options via our proprietary Drug Ratings platform, collectively solve patient cases, and participate in medical market research. For more information, visit sermo.com.
Media Contact:
Brooke Matthews
805-252-5483