In some cities in the US, hospitals are experiencing severe staffing shortages. In Atlanta, six major hospital systems in the area reported 100% to 200% increases in Covid-19 hospitalizations.
As CNN reports, “US hospitals have been dealing with their own staffing setbacks as they faced a recent surge driven by the Delta variant. Now, with Omicron spreading rapidly, hospitals are further strained.
‘The hospital is full, the ICU is full, and of course at the same time we’ve lost 20, 25% of the overall staff in the hospital due to them getting sick and having to stay home and isolate,’ Dr. Anand Swaminathan, an emergency physician in New Jersey, said Sunday.
Another problem is more people coming to the hospital seeking Covid-19 tests, he said, after waiting hours at testing sites, only for those sites to run out of tests.
‘Emergency rooms, hospitals, we’re not outfitted to do the type of testing that people need,’ he said. ‘But we also know that we’re the only option they have left.’
University of Maryland Capital Region Health on Friday announced it was activating emergency protocols due to a sharp increase in cases that overwhelmed emergency departments and field staff shortages. And in New York and New Jersey, 31 of CityMD clinics temporarily closed to “preserve our ability to staff our sites,” the company said on its website.
Early research suggests Omicron may cause less severe illness.
‘It does appear now, based on a lot of experimental evidence that we’ve gotten just in the last two weeks, that this is a milder form of the coronavirus,’ Dr. Scott Gottlieb, former commissioner of the US Food and Drug Administration, said on CBS’ ‘Face the Nation’ on Sunday. He characterized the variant as ‘more of an upper airway disease than a lower airway disease,’ which ‘is good for most Americans.’
However, Dr. Catherine O’Neal, chief medical officer at Our Lady of the Lake Regional Medical Center, said that’s not what she’s seeing at her hospital in Baton Rouge, Louisiana.
‘What we’re seeing in the hospital today is the same thing we’ve seen at the beginning of every single surge,’ she said this week. ‘To hear that Omicron is different and is not causing immense illness in people is not what we’re seeing on the ground.’
Many patients are unvaccinated and often have severe illness with pneumonia and need to be intubated. Others who are not boosted or only partially vaccinated have a flu-like illness, but most go home after a couple days, she said.
In Hennepin County, Minnesota, Dr. Andrea Rowland-Fisher, who specializes in emergency medicine, said it’s ‘a struggle’ to find hospital beds.
‘We’re having hospitals from rural Minnesota that don’t have capacity to take care of really sick people that can’t find a place to transfer their patients,’ she told CNN on Saturday. ‘And patients are clearly suffering because they can’t get the care that they need.’
Dr. Megan Ranney, an emergency room physician and associate dean at the Brown School of Public Health, said it was difficult to describe the situation in her hospital’s emergency department, with doctors and nurses ‘at the end of their rope.’
‘I have nurses and other physicians coming and kind of cry together in the break room, with a mask of course,’ she said. ‘It’s difficult to describe what it is like right now to be a health care provider and not be able to provide the care you want to give. I’ll say our hospitals are doing everything they can. There is just not enough staff and not enough space.’”
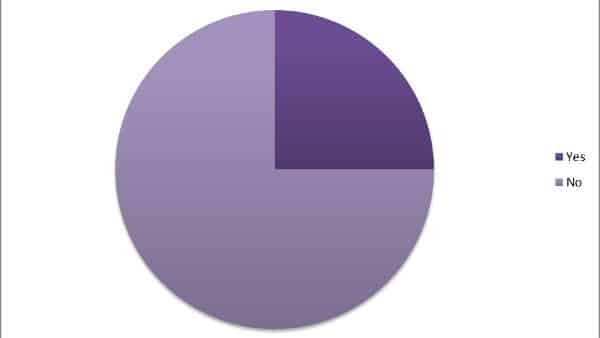
Sermo physicians from around the globe confirm they are also experiencing similar shortages. In a recent poll of about 700 physicians, 90% responded that their hospitals are dealing with staffing shortages due to Covid-19. And 81% said there is also a shortage of Covid tests and long lines for testing in their area.
Regarding the main symptoms that physicians are seeing with Covid-19 right now, 85% say there is a stark difference between patients who are vaccinated versus unvaccinated. In general, here are the main symptoms they are seeing in their patients:
- 70% say flu-like symptoms
- 42% say upper airway disease
- 40% say fever
- 39% say sore throat
- 29% say pneumonia
- 18% say loss of smell
93% of physicians say they can relate to the position that it’s difficult to be a health care provider right now and not be able to provide the care you want to give.
Below, Sermo physicians from around the world share their professional insights, perspectives, and opinions on this important topic—in their own words:
“In caring for the COVID-19 pandemic, health personnel face many challenges, among which we identified three as priorities: pandemonium, derived from the rapid progress of the pandemic and the initial chaos to respond to the emergency; the precariousness of the health system to respond to a public health problem of great magnitude, and the paranoia derived from the social response of fear in the face of the unknown.
From the beginning, health personnel in Latin American and Caribbean countries (LAC) have been the first line of care, exposed to extreme circumstances to carry out their work, higher risk of infection, long working hours, in many cases without the appropriate equipment and facing anguish, fatigue, occupational exhaustion, uncertainty, ethical dilemmas and, unusually, stigma, which manifests itself in physical and psychological violence on the part of the population.
General Practitioner, Venezuela
The vast majority of hospitalized patients in most US regions are UNvaccinated. It is SO discouraging to health workers that I have begun hearing many providers openly saying that UNvaccinated should be given lower treatment priorities as resources get more scarce since all have had (and continue to have) ready access to vaccination (like multiple vaccinations sites taking walk-ins with minimal waiting). The other interesting observation is that most US states have done little to mobilize health worker reserve volunteers (like licensed docs/RNs/therapists currently in non-clinical nonclinical jobs or recently retired). Easier to call up military & National Guard, but those resources are limited.
Anesthesiologist, U.S.
Severe symptoms are less common in vaccinated individuals.
General Practitioner, Ethiopia
In my country there is a shortage of medical personnel due to Covid, certainly, but not only that. There are several reasons why there are not enough medical personnel in hospitals, especially poor remuneration; however Covid is just the tip of the Iceberg. Regarding the variability of symptoms in vaccinated and unvaccinated, it is notorious. The vaccinated experience fairly mild symptoms compared to the unvaccinated that could even end up in the ICU/HDU.”
Otolaryngology, Nigeria
We are all experiencing hospital staffing shortages.”
Psychiatry, Italy
New strains are yet to come and more ways to avoid them have to be developed.
General Practitioner, Venezuela
We’ve seen a severe shortage of staff for a while!( nursing and doc shortage) We have seen a mixture of flu symptoms and some feel like they have a cold! Seeing symptoms with both fully vaccinated and unvaccinated!”
Plastic & Reconstructive Surgery, U.S.
Right now we have a covid outbreak in my hospital 😞 the speed of expansion of Omicron is impressive.
Pediatrics, Mexico
Everyday thousands of Sermo member physicians from diverse backgrounds and experiences exchange knowledge with each other. Sermo is the original medical social network that empowers today’s physicians. Over 1 million fully verified physicians across more than 150 countries come to our platform to talk with peers, participate in paid medical studies, solve challenging patient cases, contribute to the world’s largest database of drug ratings – and enjoy a few laughs along the way.
Interested in more? Check back any time and follow us on Facebook, Twitter, and LinkedIn for the latest and greatest in physician insights.
Are you a physician or healthcare practitioner?
Explore the many benefits of joining Sermo’s medical community and sign up for free today.