February is American Heart Month—which has become more pressing than ever during the pandemic. According to the American Heart Association, “A growing number of studies suggest many COVID-19 survivors experience some type of heart damage, even if they didn’t have underlying heart disease and weren’t sick enough to be hospitalized…Nearly one-fourth of those hospitalized with COVID-19 have been diagnosed with cardiovascular complications, which have been shown to contribute to roughly 40% of all COVID-19-related deaths…This latest twist has health care experts worried about a potential increase in heart failure.
‘Very early into the pandemic, it was clear that many patients who were hospitalized were showing evidence of cardiac injury,’ said Dr. Gregg Fonarow, chief of the division of cardiology at the University of California, Los Angeles. ‘More recently, there is recognition that even some of those COVID-19 patients not hospitalized are experiencing cardiac injury. This raises concerns that there may be individuals who get through the initial infection, but are left with cardiovascular damage and complications.’
Fonarow said these complications, such as myocarditis, an inflammation of the heart muscle, could lead to an increase in heart failure down the road. He’s also concerned about people with pre-existing heart disease who don’t have COVID-19 but who avoid coming into the hospital with heart problems out of fear of being exposed to the virus.
‘The late consequences of that could be an increase in heart failure,’ he said. ‘It is much safer if having symptoms that could represent heart attack or stroke, to come into the emergency department than to try to ride it out at home.’
Nearly one-fourth of those hospitalized with COVID-19 have been diagnosed with cardiovascular complications, which have been shown to contribute to roughly 40% of all COVID-19-related deaths.
But two recent studies suggest heart damage among those infected may be more widespread. In JAMA Cardiology, an analysis of autopsies done on 39 COVID-19 patients identified infections in the hearts of patients who had not been diagnosed with cardiovascular issues while they were ill.
Another JAMA Cardiology study used cardiac MRIs on 100 people who had recovered from COVID-19 within the past two to three months. Researchers found abnormalities in the hearts of 78% recovered patients and “ongoing myocardial inflammation” in 60%. The same study found high levels of the blood enzyme troponin, an indicator of heart damage, in 76% of patients tested, although heart function appeared to be generally preserved. Most patients in the study had not required hospitalization.
‘There’s a group of people who seem to be more affected from the cardiac point of view,’ said Dr. Mina Chung, a cardiologist and professor of medicine at the Cleveland Clinic Lerner College of Medicine of Case Western Reserve University.
But, she said, it can be difficult to identify who is at risk, or for those recovering from the virus to know if they’re having heart problems.”
Sermo physicians could not agree more.
In a recent poll of about 450 global physicians, 93% said they fear the Covid pandemic could lead to an increase in cases of heart failure; and 94% are concerned that people who have had Covid don’t understand they may be at an increased risk of heart issues. In addition, 48% of doctors have personally witnessed long-term effects on heart health in Covid patients. And 90% believe that screenings to detect cardiovascular damage should become a routine part of follow-up care for all COVID-19 patients.
Below, Sermo physicians from around the world share their professional insights, perspectives, and opinions on this important topic—in their own words:
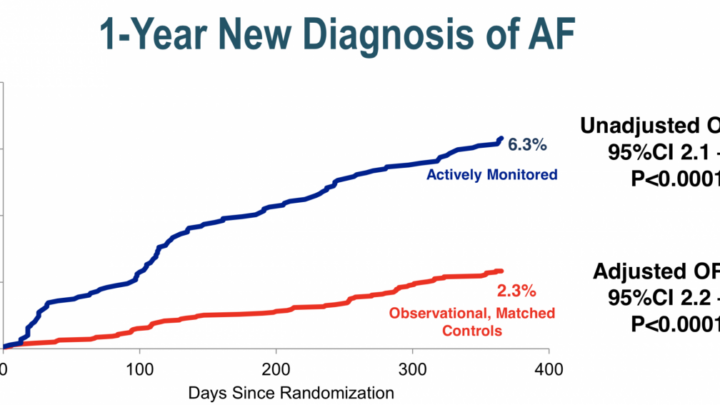
I have seen the appearance of post-COVID atrial fibrillation in patients without previous heart disease.
General Practice (GP)
Saw a 48 healthy female who was ∼ 2 months post COVID without XX. Suddenly developed pics and atypical chest pain. Found to have post COVID pericarditis.
Anesthesiology
I have done echocardiograms post infection. I don’t think insurances will pay for cardiac MRIs as it can be difficult getting an MRI.
Would stress test be of help?
Internal Medicine
I”ve seen many cardiovascular complications post-COVID– persistent sinus tachycardia, persistent chest pain of unknown etiology, and pericarditis/myocarditis–most often after mild/moderate initial infection without hospitalization. This is an area that needs continued research.
Family Medicine / Practice (FP)
Everyday thousands of Sermo member physicians from diverse backgrounds and experiences exchange knowledge with each other. Sermo is the original medical social network that empowers today’s physicians. Over 1 million fully verified physicians across more than 150 countries come to our platform to talk with peers, participate in paid medical studies, solve challenging patient cases, contribute to the world’s largest database of drug ratings – and enjoy a few laughs along the way.
Interested in more? Check back any time and follow us on Facebook, Twitter, and LinkedIn for the latest and greatest in physician insights.
Are you a physician or healthcare practitioner?
Explore the many benefits of joining Sermo’s medical community and sign up for free today.