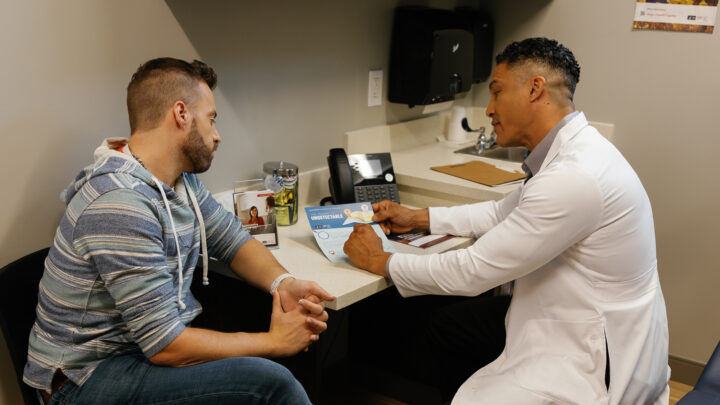
HIV care is built on having strong patient–provider relationships. Engaging in brief conversations at every office visit can help health care providers better know their patients and understand their concerns and needs, barriers to care, and ability to adhere to their treatment regimen. Patients with HIV who visit their provider regularly and take their medication as prescribed can live longer, healthier lives and prevent transmitting HIV to others.
The Centers for Disease Control and Prevention (CDC) released the HIV Care Is Prevention Toolkit, a new suite of materials offering health care providers practical tips to discuss HIV care and treatment as prevention with patients. Following are three topics highlighted in the toolkit that every provider should bring up during regular office visits to help patients with HIV adhere to their treatment regimen and maintain an undetectable viral load, stay in care, and connect with Partner Services.
1. The Benefits of HIV Treatment
HIV treatment has dramatically improved the health, quality of life, and life expectancy of people with HIV. When taken consistently as prescribed, antiretroviral therapy (ART) can suppress viral load, maintain high CD4 counts, prevent the most advanced stage of HIV, and prolong survival, all of which are important treatment goals (1,2).
ART has also transformed the HIV prevention landscape. Talking to your patients about treatment as prevention (TasP) —also known as “undetectable equals untransmittable” (U=U)—and the benefits of viral suppression is one of the best things you can do to help them stay healthy and stop HIV transmission. People with HIV who take ART as prescribed and achieve and maintain an undetectable viral load have effectively no risk of transmitting HIV to their HIV-negative sexual partners (3,4,5).
Motivate your patients with HIV to stay healthy by talking with them about the benefits of viral suppression and the prevention steps they are taking. CDC’s Starting the Conversation: HIV Treatment as Prevention brochure includes tips for starting these conversations and adopting treatment as prevention as an HIV intervention strategy in your practice.
2. Barriers to Staying in Care and Adhering to ART
Keeping patients with HIV in regular care improves their health and reduces their risk of transmitting HIV to others. Staying in HIV care and adhering to ART can be challenging, even for the most motivated patients. Poor retention in HIV care is more common in people with substance use disorders; serious mental health problems; unmet needs for housing, food, transportation, or other services; limited financial resources or health insurance; or schedules that complicate adherence to HIV medication.
Providers play an important role in retaining patients in care by emphasizing the benefits of consistent, long-term adherence to ART; monitoring and discussing patients’ needs; and linking them to support services. Read CDC’s Starting the Conversation: HIV Treatment & Care brochure to learn about common barriers patients experience and how to address them through routine conversations.
3. Partner Services Available for People Diagnosed with HIV
About 40% of new HIV infections are transmitted by people undiagnosed and unaware they have HIV (6). Offered by local or state health departments, Partner Services programs can help reduce HIV transmission by assisting patients diagnosed with HIV with locating and informing their sexual or drug injection partners of a potential exposure.
Talk to your patients about the benefits of Partner Services and the free resources they provide, including partner notification, HIV and sexually transmitted disease (STD) testing, linkage to care, risk-reduction counseling, and psychosocial support. Download CDC’s Partner Services for HIV and STDs brochure to learn more.
Access Free Tools to Start the Conversation
Order or download your HIV Care Is Prevention Toolkit today to explore brochures, posters, and more featuring the latest CDC information for you, your patients, and your practice.
For more conversation tips, follow #ExpertVoicesHIV on @CDC_HIVAIDS and www.facebook.com/cdchiv/.
[1] O’Brien WA, Hartigan PM, Martin D, et al. Changes in plasma HIV-1 RNA and CD4+ lymphocyte counts and the risk of progression to AIDS. Veterans Affairs Cooperative Study Group on AIDS. N Engl J Med. 1996;334(7):426- 431.
[2] García F, de Lazzari E, Plana M, et al. Long-term CD4+ T-cell response to highly active antiretroviral therapy according to baseline CD4+ T-cell count. J Acquir Immune Defic Syndr. 2004;36(2):702-713.
[3] Rodger AJ, Cambiano V, Bruun T, et al. Sexual activity without condoms and risk of HIV transmission in serodifferent couples when the HIV-positive partner is using suppressive antiretroviral therapy. JAMA. 2016;316(2):171-181.
[4] Bavinton BR, Pinto AN, Phanuphak N, et al. Viral suppression and HIV transmission in serodiscordant male couples: an international, prospective, observational, cohort study. Lancet HIV. 2018;5(8):e438-e447.
[5] Rodger AJ, Cambiano V, Bruun T, et al. Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study. Lancet. 2019;393(10189):2428-2438. [1] Centers for Disease Control and Prevention. Estimated HIV incidence and prevalence in the United States 2010–2016. HIV Surveillance Supplemental Report 2019;24(1). Published February 2019. Accessed January 29, 2021. https://www.cdc.gov/hiv/pdf/library/reports/surveillance/cdc-hiv-surveillance-supplemental-report-vol-24-1.pdf
[6] Centers for Disease Control and Prevention. Estimated HIV incidence and prevalence in the United States 2010–2016. HIV Surveillance Supplemental Report 2019;24(1). Published February 2019. Accessed January 29, 2021. https://www.cdc.gov/hiv/pdf/library/reports/surveillance/cdc-hiv-surveillance-supplemental-report-vol-24-1.pdf
Stay updated with the latest insights, check out more here.