For years, virtual care was touted as a convenient and equitable alternative to treat a growing population. But it had not yet been tested at scale, making up only a fraction of all healthcare interactions.
Before 2020, telehealth was mostly used by hospitals and health systems to make their specialists—located in large, central locations—more accessible across their networks. High acuity use cases such as stroke were also gaining popularity because of the technology’s ability to help care teams quickly respond to patients and remotely offer treatment recommendations, saving valuable time.
Today, virtual care has transformed healthcare delivery and proliferated into almost every specialty—behavioral health, surgical follow-up and dermatology to name a few. A Health and Human Services report found that only 840,000 Medicare visits were conducted using virtual care in 2019, compared to 52.7 million in 2020.
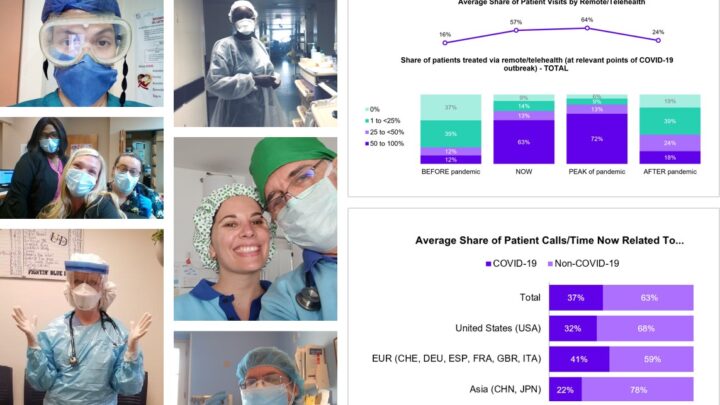
U.S. lags on telehealth, according to global physicians
Although telehealth became synonymous with healthcare during the peak of the pandemic surges, it is uncertain what is in store for this innovative care model as social distancing measures are eased. Will virtual care continue to play a large role in 2022 and beyond, or will healthcare return to mostly in-person interactions?
Is telehealth a trend or the new normal?
According to a recent Sermo RealTime survey, over 95% of US physicians conducted a telehealth visit during covid. Participants of the study were comprised of US healthcare professionals (HCPs) specializing in cardiology, critical care, dermatology, general medicine, infectious disease, internal medicine, neurology and psychiatry.
Not only did a majority of HCPs begin using telehealth, but many were forced to adapt to big—and sudden—changes to their clinical workflows without much warning or preparation.
Despite this unforeseen event, 84% of respondents would like to continue to use virtual care. Reasons vary, but accessibility and convenience were common benefits among all specialties.
- “Can be done at the convenience of patients, no need to drive or wait in the office”
- “Ease of access, low cost and helpful to patients”
- “It is a faster way to reach more patients. Patients are more comfortable speaking from their homes. Safer not to bring infectious patients into the office”
Patients also enjoyed the option to access clinical care virtually. When asked about patients’ response to virtual care, nearly three out of four HCPs reported their patients were satisfied, with only 3% marking unsatisfied (the remaining 23% remain neutral).
There is, however, a minority of physicians that do not wish to use virtual care moving forward. Of the 15% that no longer want to practice virtually, many cited their specialty and inability to physically examine the patient as the biggest drawbacks. IT issues also caused concern. Dermatologists and internal medicine physicians were the most likely to disapprove of virtual care according to the RealTime insights.
- “Hate dealing with the IT issues, especially if remote/from home”
- “It’s tough in dermatology. Usually have to have patient come in to feel confident in diagnosis”
- “No actual exam or contact with patient. A telephone call with pictures”
Overall, HCP sentiment towards telehealth was positive and many found it helpful to see more patients in a quicker amount of time. Similarly, even among those that do not wish to continue to use virtual care, they conceded some situations were appropriate and preferable, such as follow-up appointments.
Where do we go from here?
Much like the shift to remote office work, it appears virtual care is here to stay. Where appropriate, the convenience and efficiency of telehealth cannot be unlearned; many physicians and patients want virtual interactions to continue past the need for covid safety.
However, healthcare is first and foremost about quality. HCPs will always advocate for whatever is best for their patients and their unique medical needs.
That’s why, when prompted to forecast how they see healthcare operating in the future, only 14% predicted a virtual-first healthcare model, versus 74% opting for a hybrid compromise. Eleven percent believe we will return to in-person care again.
Wherever the chips fall, it is hard to imagine virtual care returning to pre-pandemic levels. These past few years demonstrated its effectiveness at scale to treat patients and extend care services. It will be interesting to see whether the name ‘virtual care’ will one day become so common that it stops being treated separately, and instead becomes just a part of care.
Use RealTime insights to spend less time doing and more time making decisions
Sermo makes it easy to quickly generate insights and engage with HCPs across the globe. RealTime surveys allow the healthcare industry to personalize insights with deep data analysis at the push of a button, informing strategy and testing new ideas without the need for expensive and time-consuming market research.
Get in touch today to request a demo and learn more by visiting sermo.com or email business@sermo.com.
Sources:
- Medicare Beneficiaries’ Use of Telehealth in 2020: Trends by Beneficiary Characteristics and Location, 2021.
- Sermo RealTime Survey (n=89), February 2022.