Impact of abortion case on physicians The US Supreme Court is taking on a key…


Impact of abortion case on physicians The US Supreme Court is taking on a key…

For parents navigating an overwhelming sea of baby products, one recommendation stands above all others:…

Consumer choice in vitamins and supplements is driven less by marketing noise and more by…

Launching a new therapy is inherently complex, particularly in categories where physician education, awareness, and…

The conversation around prescription drug costs in the U.S. is always evolving, and the introduction…

Launching a new therapy in today’s NSCLC landscape means entering one of the most competitive…

Can a doctor refuse to treat a patient for non-payment? Learn strategies for handling patients…
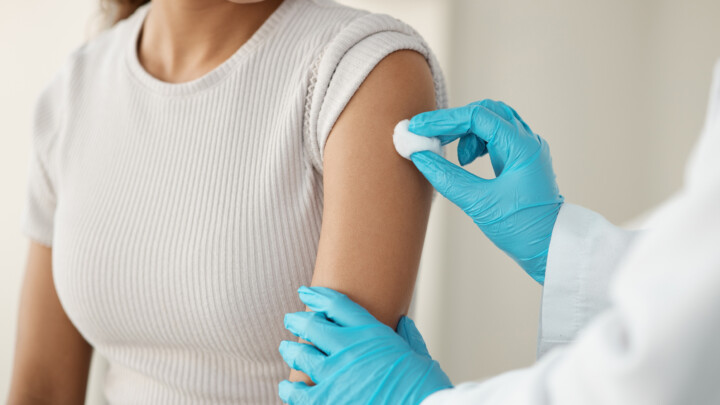
Every year, the CDC’s Advisory Committee on Immunization Practices (ACIP) sets the tone for vaccine…

Physician engagement has never been more competitive or more critical. Between packed clinic schedules, information…

Wondering if Sermo is legit? Discover how 1M+ physicians use the verified community to collaborate,…
Marketing a new medical device in today’s competitive healthcare landscape demands not only innovative strategies…
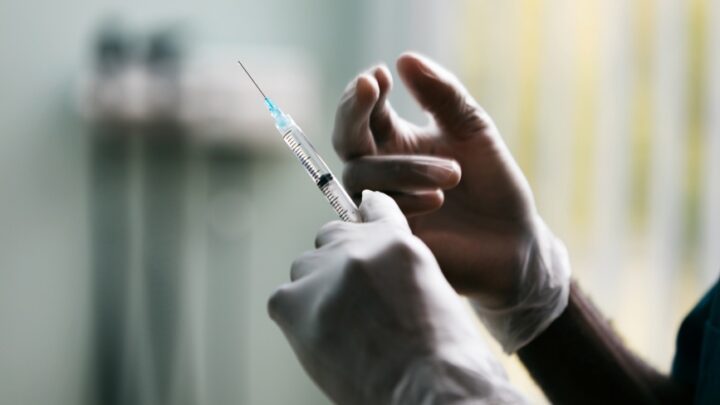
As the rates of seasonal and routine vaccinations decline, reports of increasing cases of preventable…

Medical congresses are a hub of innovation, connection, and opportunity. They’re where groundbreaking research is…